Two 2023 O’Neal NextGen Scholars have radiation oncology ties
The O’Neal Comprehensive Cancer Center (CCC) at UAB announced the 2023 class of NextGen Scholars including two awardees sponsored by Christopher Willey, M.D., Ph.D., UAB Department of Radiation Oncology Associate Vice Chair of Translational Research and Hale-Stephens ROAR Endowed Professor. Willey is also a senior scientist at the CCC.
The NextGen Scholars Awards support the training of future scientific leaders in cancer research. Manoj Kumar, Ph.D., and Lauren Nassour-Caswell are two of three scholars named this year.
“We are so thankful that the O’Neal Comprehensive Cancer Center and the Young Supporters Board selected Lauren and Manoj for the prestigious NextGen Scholars awards,” Willey said. “These funds will help support two exciting projects investigating the devastating primary brain malignancy, glioblastoma. These two named awards honor Jacob Baker and Mary Ann Harvard, who were Young Supporters Board members who succumbed to cancer. We are humbled and grateful to receive these awards.”
 Manoj Kumar, Ph.D.
Manoj Kumar, Ph.D.
The winner of the 2023 Jacob Baker NextGen Scholar Award is Manoj Kumar, Ph.D., currently a postdoctoral fellow in the UAB Department of Radiation Oncology. Kumar’s proposal investigates new ways to treat temozolomide (TMZ) and radiation-resistant glioblastomas. Surgery, TMZ chemotherapy and conventional radiation therapy are currently used to treat glioblastoma, but many forms of glioblastoma have become resistant to TMZ and conventional radiation therapy, creating a need for new treatment options. Kumar’s research will investigate the role of FLASH radiation, an innovative ultra-high dose radiation therapy with the potential to improve the therapeutic index for glioblastoma and other cancers, in treating TMZ and radiation-resistant glioblastoma.
Read moreUAB Radiation Oncology adds latest cancer-fighting technology at Acton Road clinic
The UAB Department of Radiation Oncology has launched its new TrueBeam advanced radiotherapy system at UAB Medicine’s Kirklin Clinic at Acton Road.
Clinical staff began treating cancer patients with this new cutting-edge radiation delivery system on April 3, 2023, after a three-month installation and commissioning process.
TrueBeam is Varian Medical Systems Inc.’s top-of-the-line radiotherapy technology, which can be used to treat tumors anywhere in the body where radiation treatment is indicated. It delivers a precise and fast beam of radiation to the tumor while sparing surrounding healthy tissue.
“We are proud to offer the latest cancer-fighting technology to our patients at UAB Medicine’s Kirklin Clinic at Acton Road,” said James A. Bonner, M.D., chair of the UAB Department of Radiation Oncology. “Working with the most-advanced diagnostic imaging tools and treatment systems available is what our patients expect and it allows us to provide them with the best possible care.”
In 2010, UAB was among the nation’s first cancer centers to implement TrueBeam at the Hazelrig-Salter Radiation Oncology Center in downtown Birmingham. This technology drastically reduced standard radiation treatment times from 40 minutes to less than 1 minute for select patients and opened the door to new treatment plans.
Now, patients can benefit from the advanced cancer-fighting technology at the convenient Acton Road clinic right off Interstate 459.
“It will provide patients with more options for where they can be treated with this leading-edge technology,” said medical physicist and assistant professor Jean-Guy Belliveau, Ph.D., who oversaw the commissioning of the TrueBeam at Acton Road. Patients will also benefit from shorter treatment times made possible by advances in technology including the latest safety features and automation, Belliveau explained.
Flexible treatment options, advanced imaging, high-precision dosage control, streamlined treatments, and built-in patient safety features are some of the primary benefits of TrueBeam.
Belliveau said the TrueBeam’s advanced digital automation will also allow for a more streamlined workflow for the department’s physicians, medical physicists, dosimetrists, and therapists alike. Less manual intervention will mean less downtime for maintenance and faster processes for quality assurance, he explained.
“This allows us to automate a lot of the workflows we do. It allows us to treat patients faster,” Belliveau said.
The TrueBeam replaces Varian’s Clinac EX linear accelerator at Acton Road. Belliveau said the new technology will also enhance efficiencies between the Acton Road and UAB clinics.
“If one TrueBeam is down, a patient could feasibly be treated at the other location without burdensome interventions, he explained.
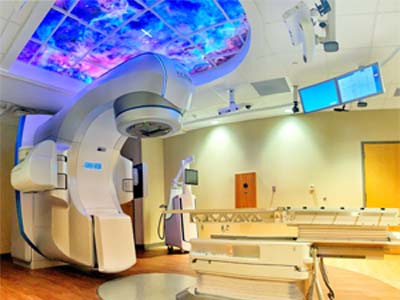
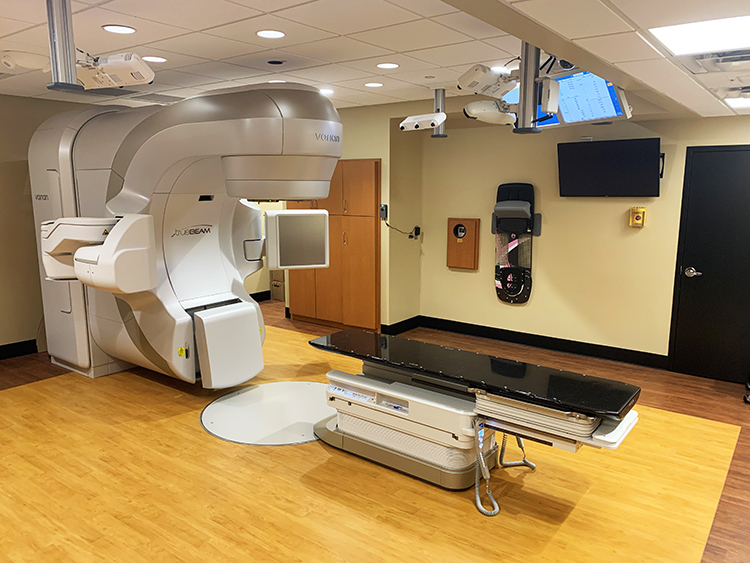 The new TrueBeam treatment room at the Kirklin Clinic at Acton Road (April 2023).
The new TrueBeam treatment room at the Kirklin Clinic at Acton Road (April 2023).
ROAR raises $388,000 for UAB Department of Radiation Oncology cancer research
 ROAR presents check from gala proceeds to Chair James A. Bonner, M.D., on April 7, 2023. Photo by Frank CarnaggioRadiation Oncology Accelerated Research (ROAR) held its 12th annual James Bond Gala: “Research to a Cure” on January 28, 2023, at The Club in Birmingham.
ROAR presents check from gala proceeds to Chair James A. Bonner, M.D., on April 7, 2023. Photo by Frank CarnaggioRadiation Oncology Accelerated Research (ROAR) held its 12th annual James Bond Gala: “Research to a Cure” on January 28, 2023, at The Club in Birmingham.
More than 350 people from the local community and beyond came out to support cancer research, raising nearly $400,000 that will go directly to fund the department’s research efforts.
“We are so impressed by the amazing support and generosity of our local community,” said ROAR President Donna Conklin. “This gala was one of our most successful to date and we are proud and honored to present a check of $388,000 to the UAB Department of Radiation Oncology.”
ROAR is a 501(c)(3) nonprofit led by volunteers with a mission to raise money for cancer research programs in the UAB Department of Radiation Oncology. Funds raised from the annual gala are matched dollar for dollar by the department and used to fund cancer research conducted by faculty and researchers. In 2022, the ROAR gala brought in $300,000 for the department.
Jeh Jeh Pruett of WBRC Fox 6 in Birmingham was the emcee for this years's gala, which included silent and live auctions, dinner and dancing, awards and recognitions, and a tribute to this year’s honoree Marilyn Mitchell Waggoner, cancer survivor, civic leader, and wife of Alabama State Senator Jabo Waggoner.
“Marilyn Waggoner is such a strong, motivating and inspirational, woman,” said ROAR Gala Chair Julie Kim.” We are truly blessed to honor such an amazing person and role model at this year’s gala.”
Waggoner, who was diagnosed with Stage 3 triple negative breast cancer in 2013, shared her personal story and message with gala attendees, “Get early detection and regular health checkups,” she said.
Waggoner and the ROAR officers presented UAB Department of Radiation Oncology Chair James A. Bonner, M.D. with the 2023 gala proceeds at a check presentation on April 7 at the Greystone Country Club in Birmingham.
“The ROAR group continues to do a remarkable job raising funds for our research program,” Bonner said. “ We are always impressed by the planning that goes into making this annual gala such an exciting and successful event for our department and our community. We cannot thank them enough for their continued support.”
Planning for next year’s gala is already underway. The 13th annual ROAR gala will be held January 27, 2024, at The Club.
 The Department of Radiation Oncology faculty members gather at the 2023 ROAR Gala. Photo by Frank Carnaggio
The Department of Radiation Oncology faculty members gather at the 2023 ROAR Gala. Photo by Frank Carnaggio
Shi appointed inaugural holder of Koikos-Petelos-Jones-Bragg ROAR Professorship
 Lewis Shi, M.D., Ph.D. Lewis Zhichang Shi, M.D., Ph.D., was appointed as first holder of the Koikos-Petelos-Jones-Bragg ROAR Endowed Professorship for Cancer Research at UAB by the University of Alabama System Board of Trustees during its Feb. 3 meeting.
Lewis Shi, M.D., Ph.D. Lewis Zhichang Shi, M.D., Ph.D., was appointed as first holder of the Koikos-Petelos-Jones-Bragg ROAR Endowed Professorship for Cancer Research at UAB by the University of Alabama System Board of Trustees during its Feb. 3 meeting.
Shi is associate professor and director of radiobiology in the UAB Heersink School of Medicine Department of Radiation Oncology. He came to UAB in 2018 from Case Western Reserve University, where he was an assistant professor, following his appointment as a research faculty member and instructor at the University of Texas MD Anderson Cancer Center, where he worked on cancer immunotherapy for a number of years with Padmanee Sharma, M.D., Ph.D., and Nobel Laureate James P. Allison, Ph.D.
At UAB, Shi has established an outstanding research program in the Department of Radiation Oncology investigating the interaction of T-cell metabolism and radiotherapy, resistance to immunotherapies, and fundamental mechanisms underlying the role of the immune system in cancer therapies.
“We were so excited when Dr. Shi elected to come to UAB even though he had offers throughout the country,” said Department of Radiation Oncology Chair James A. Bonner, M.D. “He has worked extremely hard to become a strong collaborator with numerous UAB investigators. He is truly a team player and embraces all aspects of our tripartite mission (education, research, clinical care).”
Shi has served UAB’s scientific community in numerous other ways, including as a core member of the Protocol Review Committee in the O’Neal Comprehensive Cancer Center, a reviewer for junior faculty grants, and as a faculty member for the Biomedical Scientist Training Program (PSTP).
He was recently recognized as the winner of the UAB Heersink School of Medicine’s Featured Discovery in October 2022, which celebrates important research from Heersink faculty members. Shi was chosen for his melanoma research published in Nature Communications.
Shi’s research has also been recognized through numerous awards including the Cancer Research Institute, Clinic and Laboratory Integration Program (CRI-CLIP) Investigator Award, in 2022; the V Foundation Scholar Award, in 2018; the First Immuno-Oncology Young Investigators Forum Award, in 2015; the Society of Toxicology Best Postdoctoral Publication Award, in 2009; and the Best Graduate Student in Health Sciences, Wayne Kessler Award, at Purdue University, in 2005.
Shi has also served the national scientific community as a reviewer of grants for the National Institutes of Health (NIH) and U.S. Department of Defense, and has received funding for his groundbreaking research from these national groups and many other organizations.
“I really appreciate the strong support and trust from the department by nominating me for this endowed professorship, which is a huge honor and a privilege to my group and myself. I want to thank everyone in this department and the UAB community for making me feel right at home from the get-go.” Shi said.
The Koikos-Petelos-Jones-Bragg ROAR Endowed Professorship is made possible through funding by the 501(c)(3) nonprofit organization Radiation Oncology Accelerated Research (ROAR), which is dedicated to raising funds for the UAB Department of Radiation Oncology’s research program. The endowment is named for past ROAR honorees and supporters Jimmy Koikos, Tony Petelos, Randall Earlie Jones, and Rick Bragg.
Shi will be honored at a reception hosted by the UAB Heersink School of Medicine, on April 25, 2023.
10 providers receive Patient Experience Excellence Awards
Ten providers in the UAB Department of Radiation Oncology were honored for outstanding patient care in 2022 and received a Patient Experience Excellence Award from UAB Medicine.
The award recognizes UAB providers who score an average of 95% or higher in patient care satisfaction rankings and who achieve top scores on the following metrics:
• Listened carefully
• Demonstrated care and concern
• Provided clear explanations
• Included patient in health care decisions
• Overall Care Rating, 0-10
“This is an outstanding level of performance and demonstrates your dedication to providing exceptional care and support for your patients and their families,” Reid Jones, chief executive officer of UAB Medicine, wrote in a letter to recipients. “We sincerely appreciate your service, sacrifice, and commitment to your patients, day in and day out. Providers like you help make UAB Medicine a leader in patient experience and known as an organization that patients and their families trust to provide them the best possible care.”
Radiation oncology providers recognized include:
• Drexell Hunter Boggs, M.D., associate professor
• Markus Bredel, M.D., professor
• Michael C. Dobelbower, M.D., associate professor
• John Fiveash, M.D., professor and senior vice chair
• Rojymon Jacob, M.D., professor
• Kimberly Keene, M.D., professor
• Samuel Marcrom, M.D., assistant professor
• Andrew M. McDonald, M.D., assistant professor
• Christopher Willey, M.D., professor
• Eddy Shih Hsin Yang, M.D., professor
Yang appointed to chair position at University of Kentucky
 Eddy Yang, M.D., Ph.D.Eddy Shih-Hsin Yang, M.D., Ph.D., will step into the role of chair of radiation medicine in the University of Kentucky (UK) College of Medicine on Feb. 1, 2023.
Eddy Yang, M.D., Ph.D.Eddy Shih-Hsin Yang, M.D., Ph.D., will step into the role of chair of radiation medicine in the University of Kentucky (UK) College of Medicine on Feb. 1, 2023.
Dr. Yang most recently served as professor and vice chair for translational sciences in the University of Alabama at Birmingham (UAB) Department of Radiation Oncology. He also served as the deputy director and associate director for precision oncology at the UAB Hugh Kaul Precision Medicine Institute, and was co-leader of the Experimental Therapeutics Program at the O’Neal Comprehensive Cancer Center at UAB.
Yang came to UAB in 2010 after completing residency at Vanderbilt University. As a physician scientist, Yang was instrumental in creating an exceptional educational research program that has allowed UAB to train the next generation of physician scientists in the field of radiation oncology.
Yang was also the Radiation Oncology Accelerated Research (ROAR) Southeast Cancer Foundation Endowed Chair since 2012.
During the 12th annual ROAR gala on Jan. 28, 2023, UAB Department of Radiation Oncology Chair James Bonner, M.D., honored Yang with the Radiation Oncology Scholar Award for his dedication and devotion to the advancement of the science of radiation oncology during his impactful practice at UAB Medicine.
At UK, Yang will continue his research work in the areas of genitourinary, breast, and head and neck cancers, and will hold the distinction of Markey Cancer Foundation Endowed Chair in Radiation Medicine.
Shi wins Cancer Research Institute grant to tackle immunotherapy resistance
 Lewis Shi, Ph.D. Lewis Zhichang Shi, Ph.D., Associate Professor in the UAB Department of Radiation Oncology, has been awarded a Clinic and Laboratory Integration Program (CLIP) grant from the Cancer Research Institute (CRI).
Lewis Shi, Ph.D. Lewis Zhichang Shi, Ph.D., Associate Professor in the UAB Department of Radiation Oncology, has been awarded a Clinic and Laboratory Integration Program (CLIP) grant from the Cancer Research Institute (CRI).
CLIP grants provide up to $200,000 over a two-year period to support investigators like Shi who are studying critical topics at the intersection of laboratory and clinical research, known as translational research.
Shi’s CLIP project is titled, “Discovering and targeting tumor-intrinsic metabolic checkpoints to overcome immunotherapy resistance.”
“This CRI grant will allow me to tackle a major mechanism of resistance to immunotherapy in colorectal cancer, melanoma, and bladder cancer, a pressing unmet medical need,” Shi said.
Shi’s recent research on immunotherapy resistance in melanoma patients, “Selective suppression of melanoma lacking IFN-γ pathway by JAK inhibition depends on T cells and host TNF signaling,” was recently published in Nature Communications and recognized as the latest “Featured Discovery” by the UAB Heersink School of Medicine. Shi is also a scientist in the O’Neal Comprehensive Cancer Center at UAB.
Read Shi’s CLIP investigator profile here.
UAB Radiation Oncology offers adaptive therapy for breast cancer patients
UAB Radiation Oncology is excited to announce its new Stereotactic Body Radiation Therapy program for breast cancer patients using adaptive radiotherapy technology.
The majority of women who present with early-stage breast cancer are a candidate for a lumpectomy, which is removal of the breast tissue and sparing of the uninvolved breast. Traditionally, four to six weeks of radiation therapy to the whole breast was required afterward to decrease the chance that the tumor would recur. More recently, for appropriately selected patients, a shorter course of partial breast radiation allows treatment to be completed over five courses. In addition, less of the normal breast is exposed to radiation, which reduces short- and long-term side effects compared to patients getting whole breast radiotherapy.
UAB Department of Radiation Oncology Associate Professor Hunter Boggs, M.D., recently published UAB’s experience with using sterotactic body radiotherapy (SBRT), which is a precise form of radiation treatment to deliver five treatments to the lumpectomy cavity.
“The ability to reduce the surrounding dose to the uninvolved breast resulted in excellent short-term cosmetic outcomes in our study. We are still collecting data regarding long-term side effects,” said Boggs. “However, one of the issues that we would find is that the fluid collection, called a seroma, left at time of lumpectomy will shift and often shrink as the treatments progressed. The area of breast tissue surrounding the seroma is the target area of treatment for partial breast irradiation after a lumpectomy. If we could find a way to shrink our daily treatments to better pinpoint and target the fluid collection, we would be able to further decrease the amount of normal breast treated. We know that reducing the amount of radiation to the uninvolved breast results in improved side effects from treatment.”
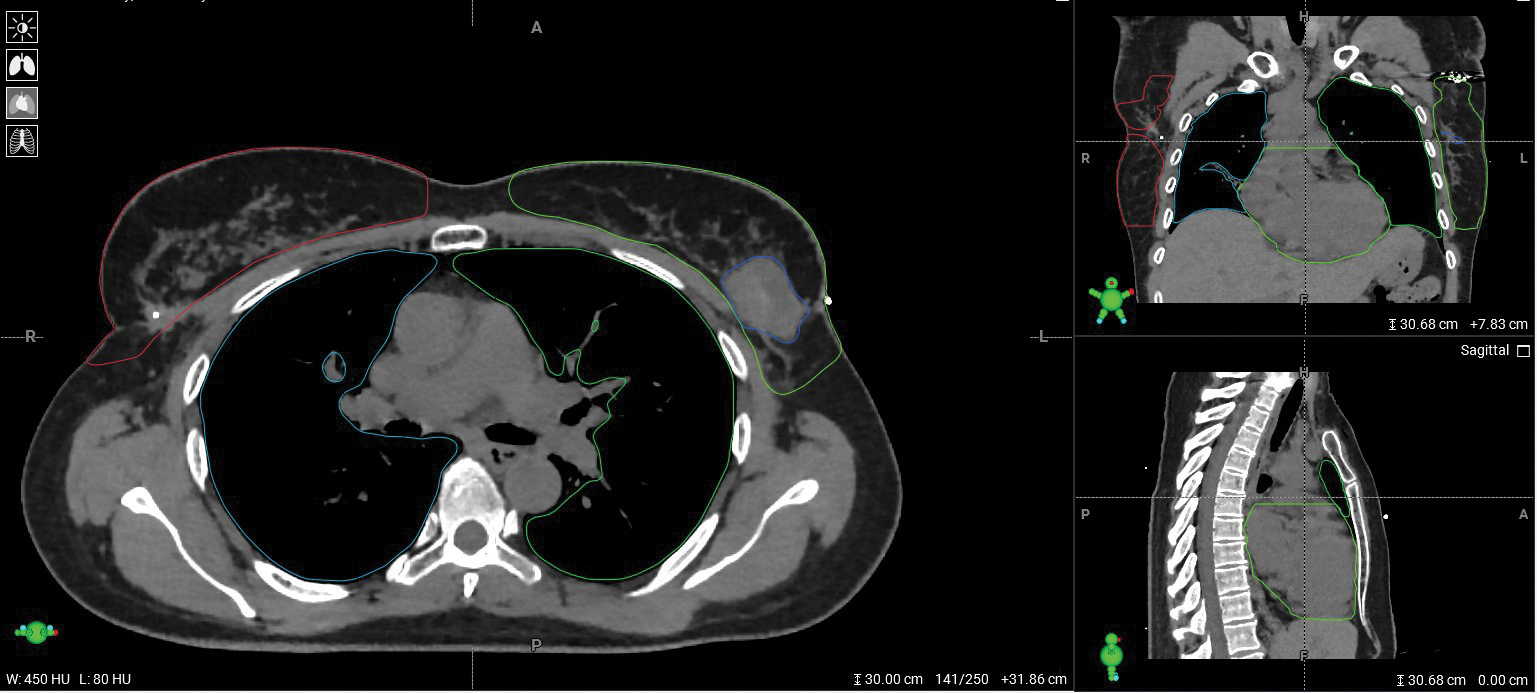 Using an advanced imaging algorithm, Ethos is able to visualize the patient anatomy of today and create a custom radiation plan for that day. This is an example of the imaging utilized by the Ethos system with the seroma outlined in blue.
Using an advanced imaging algorithm, Ethos is able to visualize the patient anatomy of today and create a custom radiation plan for that day. This is an example of the imaging utilized by the Ethos system with the seroma outlined in blue.Adaptive Therapy with Ethos
Enter adaptive therapy, utilizing a linear accelerator system called Ethos by Varian, which was first implemented by the radiation oncology department in August 2021. Ethos is a first-of-its-kind treatment machine that uses advanced imaging and an artificial intelligence (AI) system to assist in plan creation and delivery. “The Ethos is a complete game changer for radiation oncology,” said Assistant Professor Dennis Stanley, Ph.D., lead physicist for the adaptive program. “Utilizing the advanced features of the Ethos allows us to better target tumors but, more importantly, better protect healthy tissues like the breast and heart. With this system we can treat your tumor as it is right now.”
“We draw out the lumpectomy cavity at time of the planning scan,” Boggs explained. “With nonadaptive therapy, we were locked into treating the same volume regardless of how the breast changes from day-to-day. However, with adaptive therapy, we can scan and redraw the lumpectomy cavity in real time while the patient is laying in the treatment position. If the breast and lumpectomy cavity are sufficiently different than our initial scan, we can replan immediately and see if our new plan will result in less dose to the normal breast and other critical organs nearby such as the heart and lung. We do this before every treatment."
According to Boggs and Stanley, UAB is the first institution in the world to treat patients with partial breast stereotactic techniques using daily adaptive replanning. “We have treated a handful of patients using this technique and we plan to examine our cosmetic outcome information over the coming months and years,” said Boggs.
“From a technical standpoint, this treatment option offers tremendous advantage, especially for our breast cancer patients; we look forward to developing this treatment technique even further,” said Stanley.
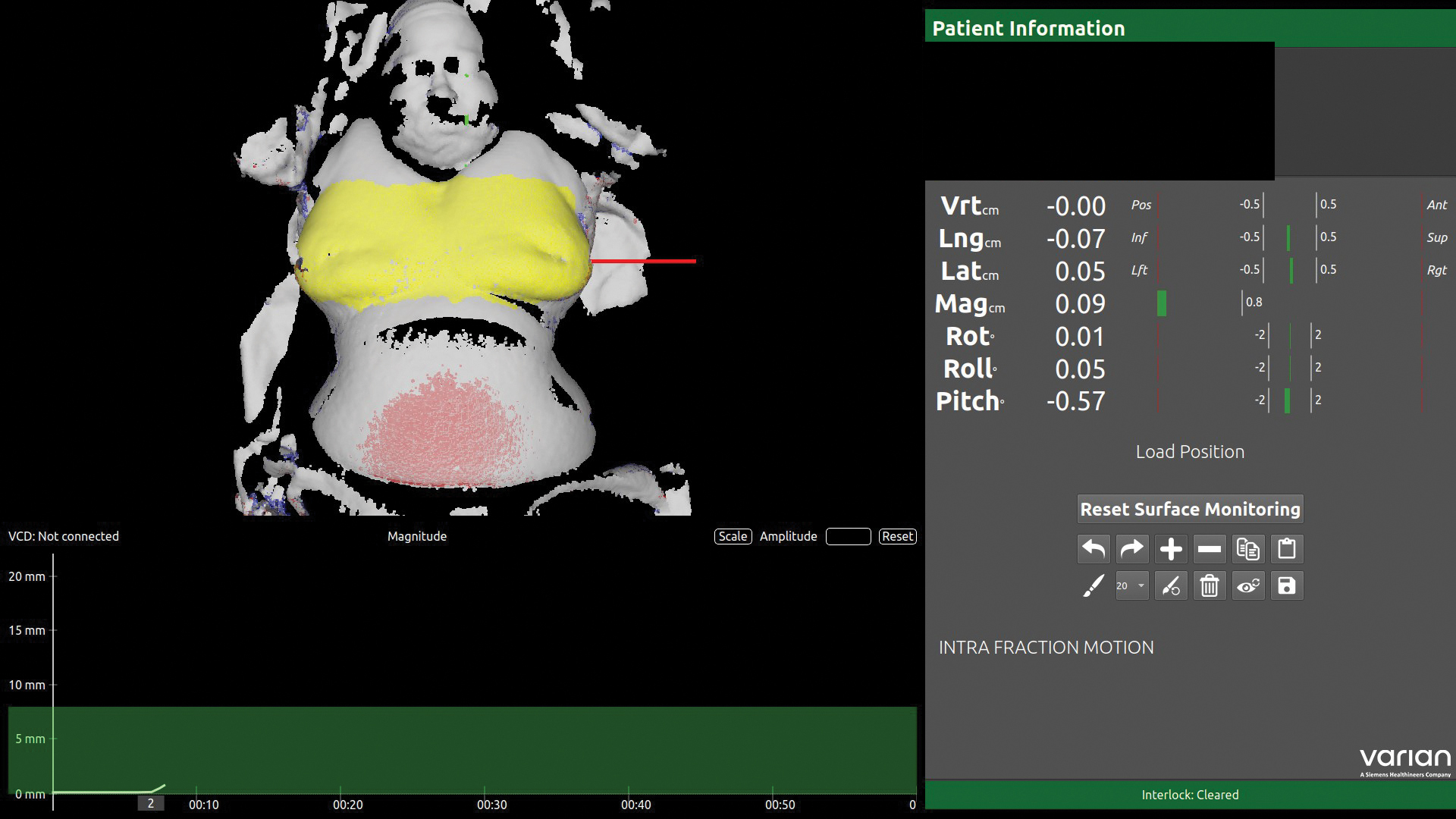 Along with the advanced treatment techniques, Ethos utilizes an optical-based surface imaging system, called IDENTIFY, to verify patient positioning and monitor patient movement.
Along with the advanced treatment techniques, Ethos utilizes an optical-based surface imaging system, called IDENTIFY, to verify patient positioning and monitor patient movement.
Next Steps
Regarding next steps, Drs. Boggs and Stanley and the breast radiation oncology team are interested in exploring reducing the number of treatments required for a partial breast treatment.
“We have opened a clinical study examining the use of partial breast radiation delivered in a single treatment,” Boggs says. “We think that this will be an attractive option for patients who are looking to reduce the physical burden of coming in for a number of treatments. The adaptive technique will be perfect for this type of treatment given the need to precisely understand the shape of the lumpectomy cavity as well as the breast position prior to the single course of treatment.”
For more information about adaptive radiation therapy for partial breast irradiation, please contact 205-934-5670.
Research reveals potential targets for therapeutic development for glioblastoma
UAB Department of Radiation Oncology researchers have identified potential targets to help overcome therapy-resistant tumors in patients with glioblastoma (GBM), the most common and devastating form of primary brain cancer. 
UAB Department of Radiation Oncology Hale-Stephens ROAR Endowed Professor Christopher Willey, M.D., Ph.D., with co-authors, recently published the research, “An in vivo model of glioblastoma radiation resistance identifies long noncoding RNAs and targetable kinases” in the peer-reviewed journal JCI Insight.
“This project is focused on a real clinical problem we face in treating glioblastoma and that is acquired therapeutic resistance,” Dr. Willey said.
The current standard of care for this disease is surgery, if possible, followed by radiation and chemotherapy.
“Unfortunately, the tumor pretty much universally recurs and the median survival is only 15 months from diagnosis,” Dr. Willey said.
While there is much research on radiation resistance for GBM, Dr. Willey said most tumor models used in studies have never actually seen therapy before. “There is a lack of acquired therapeutic resistance models, particularly radiation, and we sought to improve upon that,” he said.
The new article explains how researchers used a patient-derived xenograft program, or PDX, for this disease to generate some acquired radiation resistance models that they then profiled to try to identify potential pathways of resistance.
Researchers were successful in generating phenotypically and molecularly diverse models of GBM tumor recurrence, particularly related to radiation.
They also identified alterations in long noncoding RNA transcripts (lncRNAs) in the acquired radiation-resistant PDX lines, which were associated with several gene expression signatures (e.g., cell cycle, stemness, and DNA damage response) suggesting that lncRNAs could potentially regulate pathways that lead to radiation resistance.
“And particularly important, kinomic profiling from these models reveals potential targets for therapeutic development for GBM recurrence,” Dr. Willey said.
Watch Dr. Willey’s Author's Take video for JCI Insight. Look for a summary of this article in the September 2022 "JCI This Month" print digest.
Co-authors from the UAB Heersink School of Medicine include: Christian T. Stackhouse, Department of Radiation Oncology and Department of Neurosurgery; Joshua C. Anderson, Nicholas J. Eustace, Chuan Xing, Hasan Alrefai, Kevin J. Lee, and Eddy S. Yang, Department of Radiation Oncology; Zongliang Yue, Jelai Wang, and Jake Y. Chen, Informatics Institute; Catherine P. Langford and G. Yancey Gillespie, Department of Neurosurgery; Fady M. Mikhail, Department of Genetics; Ryan E. Bash and C. Ryan Miller, Division of Neuropathology, Department of Pathology; and Anita B. Hjelmeland, Department of Cell, Developmental, and Integrative Biology.
Other co-authors include: Xiangqin Cui, Emory University Rollins School of Public Health Department of Biostatistics and Bioinformatics; James R. Rowland IV, The Ohio State University Department of Physics.
New research identifies strategy to overcome ICB resistance in melanoma patients
UAB Department of Radiation Oncology Chair James A. Bonner, M.D., and Associate Professor Lewis Zhichang Shi, M.D., Ph.D., recently published research with new implications for treating melanoma patients.
The article, “Selective suppression of melanoma lacking IFN-γ pathway by JAK inhibition depends on T cells and host TNF signaling” published in Nature Communications discusses the pressing issue of resistance to immunotherapy drugs called immune checkpoint blockers (ICBs) in melanoma patients.
Immune checkpoints are a normal part of the immune system that occur when proteins on the surface of immune cells (T cells) bind with their partner proteins on other cells such as tumor cells. This binding signals to the T cells not to destroy the cancer cells. ICBs work by blocking the binding, which allows the T cells to kill the cancer cells.
Melanoma, the most serious form of skin cancer, was largely considered incurable prior to the era of ICBs, yet accumulative data show only a subset of melanoma patients actually benefit from ICBs, limiting their clinical use.
Initial research from Dr. Shi (while working at The University of Texas MD Anderson Cancer Center with Padmanee Sharma, M.D., Ph.D., and Jim Allison, Ph.D.) on therapeutic resistance to ICBs in melanoma cells identified a lack of certain signaling genes (IFN-γ). Strategies to overcome this mechanism of resistance have remained largely unexplored until now.
Upon relocating to UAB in 2018, the Shi group, teaming up with Bonner group and other research teams within the department, set out to uncover therapeutic targets to treat ICB-resistant melanomas lacking functional IFN-γ signaling. They started by creating a new melanoma model that lacked IFN-γ signaling and was completely resistant to ICBs.
Researchers demonstrated that melanomas lacking IFN-γ signaling have reduced infiltration and effector function of tumor-infiltrating T cells (TILs) but exhibit an unusually active mTOR-JAK1/2 axis, a pathway essential for cell survival.
Their findings led them to employ Ruxolitinib (Ruxo), an FDA-approved JAK1/2 inhibitor to treat myeloproliferative neoplasms (MPN), a type of blood cancers. They found inhibiting activated JAK1/2 with Ruxo induced selective suppression of IFNγR1KO melanomas, in a precision medicine fashion.
“Since Ruxo is clinically approved, our study justifies further testing of Ruxo in patients with advanced melanoma that are resistant to ICBs, particularly those with impaired IFN-γ signaling,” Dr. Shi said. “We are actively soliciting clinical interests in exploring JAK1/2 inhibition as a strategy to overcome ICB resistance in melanoma patients, a pressing unmet medical need.”
Read the full article with results in Nature Communications.
Read Dr. Shi’s related “Behind the Paper” post, “Overcoming immunotherapy resistance in melanoma defective of IFN-g signaling” in the online Nature Portfolio Cancer Community.

Breast cancer awareness in action
 October is Breast Cancer Awareness Month, which means you’re probably seeing ribbons and the color pink on almost every corner. This “pinkwashing” in October serves as a constant reminder of the disease. For those affected by breast cancer, it also makes October a hard month to emotionally navigate.
October is Breast Cancer Awareness Month, which means you’re probably seeing ribbons and the color pink on almost every corner. This “pinkwashing” in October serves as a constant reminder of the disease. For those affected by breast cancer, it also makes October a hard month to emotionally navigate.
Increased awareness is crucial for the fight against breast cancer, but it needs to extend beyond the flood of pink ribbons in October. Here are some ways you can join us in turning Pinktober awareness into year-round action:
-
Support survivors and those affected by checking on them to see how they are faring with the increased reminders.
-
Honor the many lives affected by reminding your loved ones (and yourself) to schedule and keep regular GYN appointments that include a clinical breast exam.
-
Remain breast-health aware throughout the entire year by educating yourself on the signs and symptoms of breast cancer, along with the proper technique for conducting regular self-breast exams.
UAB Radiation Oncology is proud to be a part of the National Cancer Institute-designed O'Neal Comprehensive Cancer Center at UAB and a breast cancer program that ranks among the best in the nation. Patients who come to UAB Medicine for breast cancer treatment have access to the full array of specialists within our system, along with a wide range of patient resources to support you physically and emotionally. For more information on UAB Medicine breast cancer patient care and resources, visit https://www.uabmedicine.org/patient-care/conditions/breast-cancer?medallia=occ-survey.
Clinical trial evaluating a novel, non-invasive radiation treatment for ventricular tachycardia refractory to medication and catheter ablation
 The UAB Departments of Radiation Oncology and Cardiology are looking for patients with ventricular tachycardia (VT) not controlled by medications and catheter ablation.
The UAB Departments of Radiation Oncology and Cardiology are looking for patients with ventricular tachycardia (VT) not controlled by medications and catheter ablation.
The trial will allow patients suffering from VT despite standard of care regimens to undergo non-invasive cardiac radioablation (CRA; a type of stereotactic body radiotherapy) to the area of the heart responsible for their symptoms. Stereotactic body radiotherapy is delivered with a device called the linear accelerator, which is primarily used to treat patients with cancer.
UAB is one of the first centers in the U.S. to obtain a Food and Drug Administration (FDA) investigational device exemption for use of the linear accelerator in this capacity on a phase I/II trial.
The study is being conducted in collaboration with the Washington University School of Medicine in St. Louis, a center which pioneered this promising technique in the U.S.
For more information on the RAD 1901 trial, please contact Adelyn Gillon, clinical research coordinator, at 205.975.3019 or agillon@uabmc.edu.