Case History
A 35-year-old G3 P2022 mother was transferred to UAB for induced vaginal delivery at 37 weeks due to intrauterine fetal demise. Post-mortem evaluation demonstrated a mildly microcephalic but otherwise nondysmorphic, hydropic female fetus. The brain weighed 201 g (268-412 g expected). There was ventriculomegaly, periventricular necrosis, calcification and hemorrhage.
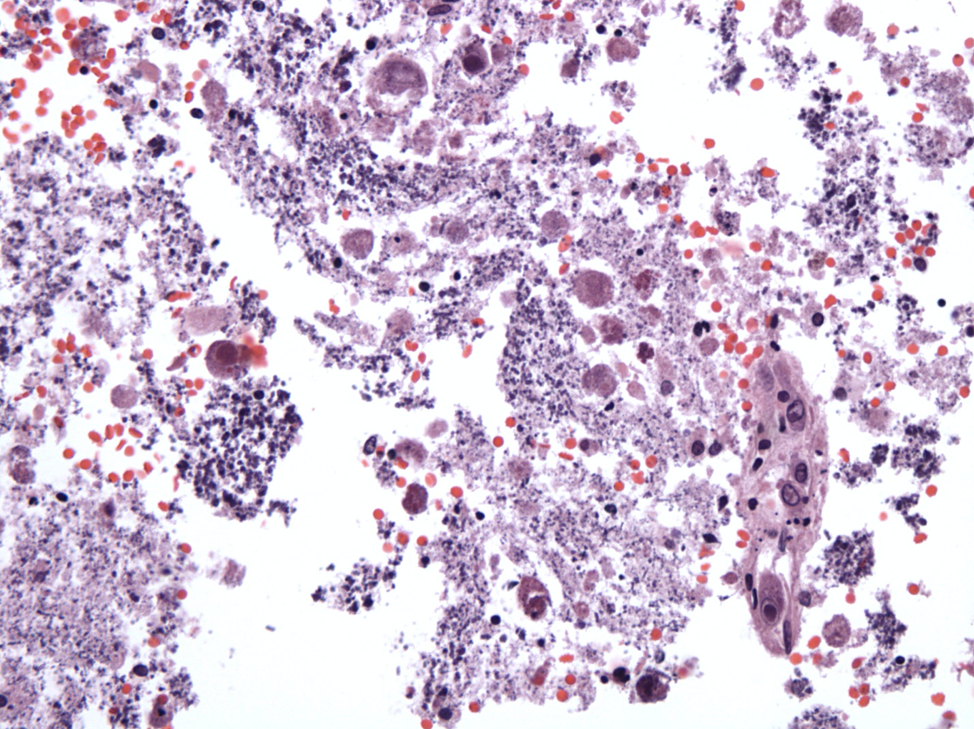
Based on the above image, what is the most likely diagnosis?
- Intrauterine stroke
- HSV infection
- Germinal matrix bleed
- CMV infection
ANSWER: D: CMV Infection (congenital)
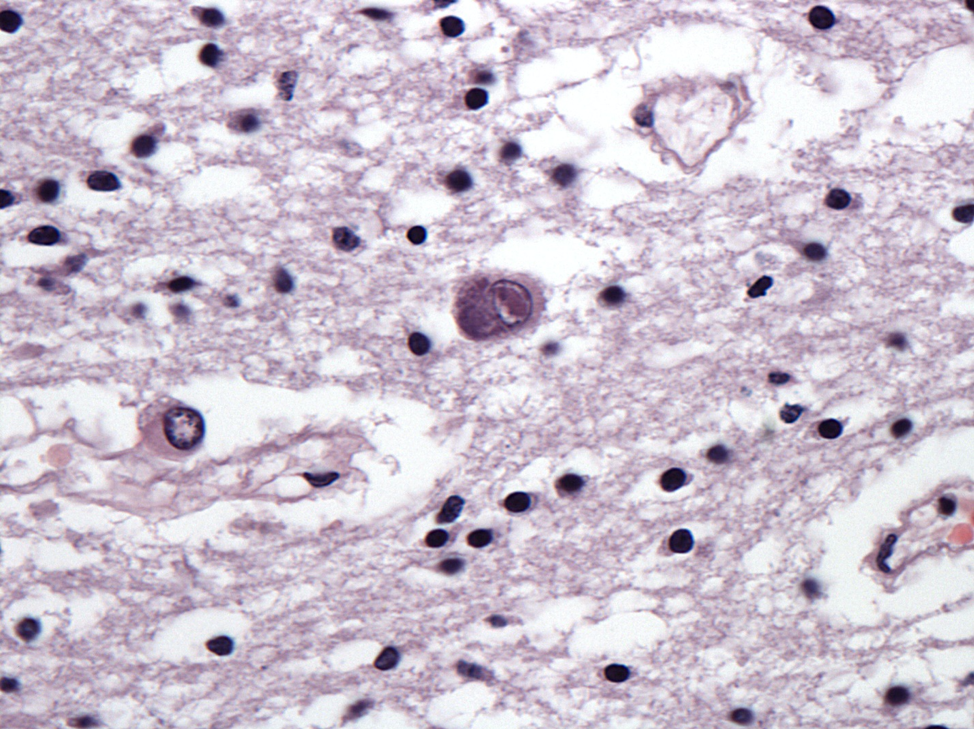
This is a characteristic case of gestational CMV infection. Morphologic changes of the first image include markedly enlarged, infected cells, disruption of the periventricular neuropil and granular calcifications. The second image demonstrates a classic CMV-infected cell exhibiting enlarged nucleus, intranuclear viral inclusion, as well as an ill-defined intracytoplasmic viral inclusion. CMV is the only common viral disease characterized by both intranuclear and intracytoplasmic viral inclusions.
Case contributed by: James Hackney, M.D., Associate Professor, Neuropathology